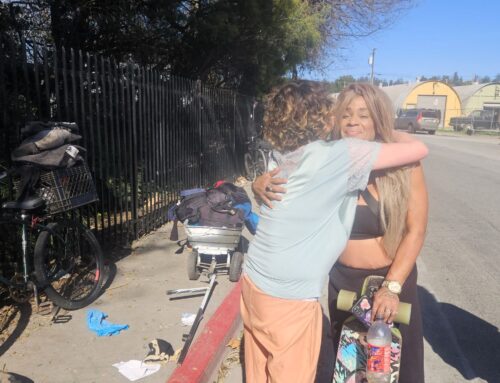Santa Cruz County Behavioral Health serves many clients in the Emeline Complex at 1400 Emeline Ave. in Santa Cruz. (Michael Warren Mott — Santa Cruz Local)
SANTA CRUZ >> Santa Cruz County’s Behavioral Health Division has been short staffed for several years, which has worsened patient outcomes and led to overworked mental health workers and increased county costs, according to a recent report by the Santa Cruz County Civil Grand Jury.
The report “urgently recommends” that the Behavioral Health Division increase its staff to meet demand, as well as increase the capacity of its crisis stabilization program, make the Mobile Emergency Response Team 24 hours and improve services for Latinos, the unhoused and people involved with the criminal justice system.
“We all were surprised by how dire the staffing shortage is,” said Terry Eastman, the Civil Grand Jury foreperson. “More than any other piece, that’s making it hard to provide mental health services in this county.”
- The Behavioral Health Division is the primary provider of mental health and addiction-related services for adults and children who have low incomes or lack private health care coverage.
- About 37% of its clients are not housed, the report states.
- About 2 out of 3 homeless residents of Santa Cruz County experience chronic substance abuse, according to a 2022 point-in-time count survey of 333 people.
The Behavioral Health Division was about 26% understaffed and lacked more than 74 full-time equivalent positions in March, according to the report. About one-third of its services are provided by county employees and two-thirds of its services are provided by private contractors, according to a 2022 quality review.
The county’s crisis care takes place at the Santa Cruz Psychiatric Health Facility at 2250 Soquel Ave. in Santa Cruz. It is often closed to new admissions because of a lack of bed capacity and staff. Clients are often referred to hospital emergency rooms or facilities outside the county, the report stated.
The Santa Cruz Psychiatric Health Facility, or Telecare, is privately run. It has 16 beds and should have about 135 beds based on the county’s population of roughly 270,000 people, according to a 2016 report by the nonprofit Treatment Advocacy Center.
“Patients and families report delays in receiving needed services, or inability to find services when they need them,” the report states. “Homeless people and those involved with the criminal justice system have unique needs and barriers, and experience long wait times to access [Behavioral Health Division] services,” according to the report.
Staff shortages
The Behavioral Health Division has four subdivisions: Adult Mental Health, Children’s Mental Health, Substance Use Disorders and Quality Improvement. As of the report’s March data, the division has staffing shortages in:
- 31% staffing vacancy rate in crisis support.
- 27% vacancy in Adult Mental Health.
- 29% vacancy in Substance Use Disorders.
- 25% vacancy in administration.
- 24% vacancy in Children’s Mental Health.
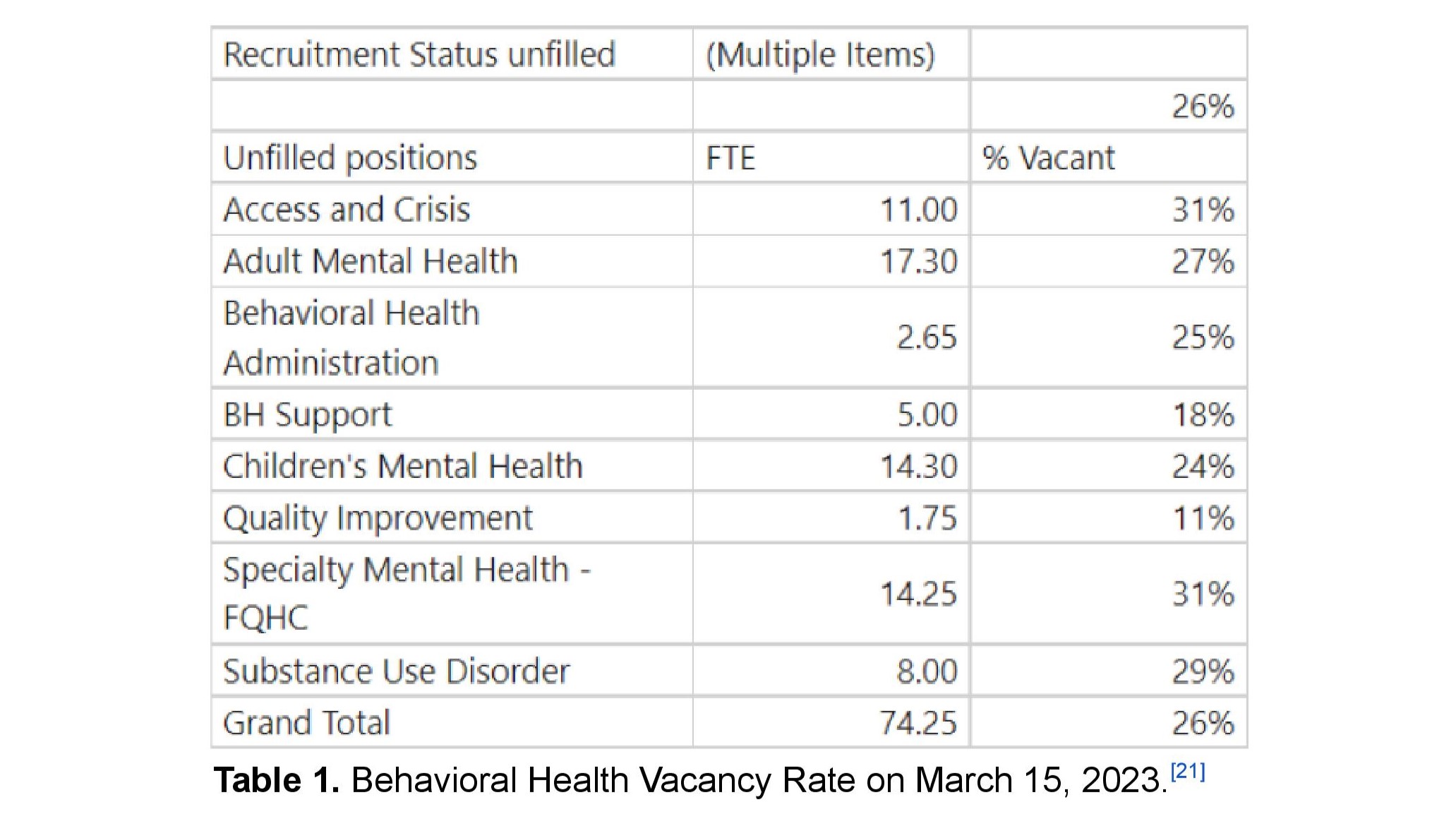
Santa Cruz County’s Behavioral Health Division is facing major staffing shortages, per a recent report by the Santa Cruz County Grand Jury. (Santa Cruz County Civil Grand Jury)
The Civil Grand Jury is a group of volunteers who research and investigate local government and publish reports to try to improve public systems.
In March, leaders of the Behavioral Health Division released a draft of its Mental Health Services Act FY 2023-2026 Three Year Plan and FY 2023-2024 Annual Update, which included input from community members concerned about staff shortages.
The Three Year Plan reported that many people use crisis services often because they don’t receive adequate or consistent step-down services outside of crises. Patients and families often had service delays or could not find services when they needed them, the plan stated. People without housing often had long wait times. Due to a lack of bilingual staff and culturally responsive services, Latinos were served less than any other ethnic group, the plan stated.
Major service gaps in the Three-Year plan became the Civil Grand Jury’s focus of investigation.
The Grand Jury found that nearly all of the goals set by Behavioral Health for itself in 2021-2022 were not met. Goals not met included services access, response times and cultural responsiveness, the report said.
“It has been difficult to hire licensed staff, social workers, therapists, psychologists and nurse practitioners with mental health specializations,” said Karen Kern, deputy director of the Behavioral Health Division. “Because of that, it has been very difficult to meet the needs of the community.”
Kern said the staff shortages are not uncommon. “It’s not just us, it’s a national crisis. Forty-nine percent of Americans live in an area with a mental health workforce shortage,” Kern said, based on research by the National Institute for Healthcare Management Foundation.

Mental health services are available at the Emeline complex. (Michael Warren Mott — Santa Cruz Local)
Potential solutions
The Grand Jury offered several recommendations:
- Speed up a hiring process that often takes one to three months. The County Personnel Department is trying to halve that time.
- Raise salaries and add hiring bonuses and other incentives like loan repayment and workforce tuition.
- Increase capacity of outpatient care and psychiatric beds for clients in crisis, which may include planning for another psychiatric care facility.
- Operate Mobile Emergency Response Teams for adult and youth 24 hours rather than 8 a.m. to 5 p.m. weekdays because of the staff shortage.
- Improve bilingual and bicultural outreach to the Latino population, as well as see whether staff who speak any language other than Spanish should receive more pay.
- Ensure a smooth transition for youth treatment until a new facility in Live Oak is finished.
- Request more funding for non-crisis services.
Santa Cruz County spokesperson Jason Hoppin said that lengthy hiring times are partly because of civil service rules.
Kern said the COVID-19 pandemic exacerbated problems. Telehealth made it difficult for some practitioners, including some with children who were doing online learning.
Kern said the report validated some changes that Behavioral Health has been considering for about 18 months. Behavioral Health is working with the Personnel Department to speed up hiring.
The report noted a senior mental health specialist is paid $10,000 more in Santa Clara County than in Santa Cruz County. A similar position in Santa Cruz County has not received an applicant in about two months, Kern said.
High housing costs have been a factor for why people decline positions in Santa Cruz County, Kern said. Many staff members live in Hollister and Los Banos so they can afford housing.
Kern also acknowledged that salaries are “not as competitive as we could be.”
A few potential solutions are in the works.
- Recruitment is now continuous and not time limited.
- Salaries have been raised for hard-to-hire positions. Recruiters have been used and changes have been made to social media advertising.
- To address the limited client capacity, the county is adding a new facility in Live Oak for children and youths that is expected to open in 2024 or 2025. An interim solution is in the works with Watsonville Community Hospital, Kern said.
- Per patient costs are higher here because of the high use of crisis services, Kern said. Behavioral Health is working on building more lower-level services to reduce reliance on the crisis system. A new facility for South County services, the Sí Se Puede Behavioral Health Center at 191 Miles Lane in Watsonville, is also being built. It is expected to add 30 more beds and be operated by Encompass Community Services.
Next steps
Leaders of the Behavioral Health Division are expected to discuss a proposed Crisis Now model at the Santa Cruz County Supervisors’ June 27 meeting. It includes a 24-hour crisis team, a suicide hotline call center and mental-health crisis response without law enforcement.
Some residents have asked for more crisis solutions that don’t include law enforcement since 2016. That year, two Santa Cruz County residents were killed by law enforcement officers during separate mental health crises.
The Civil Grand Jury also pointed to a lack of regular competitive analysis around salaries and a lack of recognition in staff shortages in the county’s Personnel Department.
The Santa Cruz County Supervisors are required to respond to the Civil Grand Jury report by Sept. 11.
The Civil Grand Jury also invited responses from County Administrative Officer Carlos Palacios, the county’s Mental Health Advisory Board, and the directors of the Behavioral Health Division, Health Services Agency and county Personnel Department.
Questions or comments? Email [email protected]. Santa Cruz Local is supported by members, major donors, sponsors and grants for the general support of our newsroom. Our news judgments are made independently and not on the basis of donor support. Learn more about Santa Cruz Local and how we are funded.
Michael Warren Mott is a graduate of UC Santa Cruz and Columbia University's School of Journalism. He has worked for newspapers across California.